By Polly Swingle, PT, GCS, CEEAA, and Brian Paulson, CPO
Foot drop is a potentially painful—and even disabling—condition where an individual has difficulty raising (or a complete inability to raise) the front of the foot. Foot drop—also referred to as dropped foot or drop foot—is caused by a damage or impairment to the muscles and nerves responsible for lifting the foot. The resulting weakness or paralysis leads to characteristic symptoms that most obviously manifest in an altered gait. Because individuals suffering from foot drop cannot properly lift their foot, they may drag their toes on the ground while walking. To avoid this potentially painful and dangerous impairment (which can damage the foot and increase the risk of falling), foot drop patients may utilize a “steppage gait,” a common compensation tactic where they lift their knee(s) higher in a marching-style walk or swing their leg(s) outward.
Causes of Foot Drop
It is important to understand foot drop is not a disease; it is a symptom. There are several types of damage or diseases that can weaken nerves and/or muscles and lead to foot drop, but the three most common are an injury to the peroneal nerve that controls the muscles responsible for lifting the foot; muscular compromise due to a disorder such as amyotrophic lateral sclerosis (ALS) or muscular dystrophy; and neurological conditions such as multiple sclerosis (MS) or stroke.
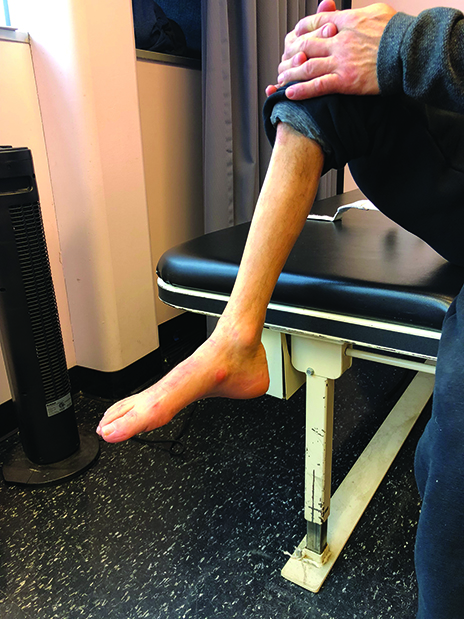
Top: Patient has a diagnosis of Cauda Equina injury due to a lumbar discectomy that had complications, and resulted in loss of his distal muscles controlling the ankle. The intervention for this injury is physical therapy for strengthening the intact muscle above the ankle, as well as balance activities and a solid AFO. Bottom: Patient walks with an AFO which supports his ankle. While the loss of muscles in his lower leg will be permanent, the orthosis will stabilize the foot and aid in walking.
Treatment Options
There are four basic categories of treatment options for foot drop. Because successfully treating foot drop almost always depends on addressing/correcting the underlying cause of the condition, the best course of treatment and therapeutic care can vary significantly from one patient to the next.
Treatment options include the following:
Surgical intervention
Surgical treatment options can be effective for foot drop patients whose condition has been caused by physical damage to nerves or muscles. A herniated disc, tumor, or other spinal condition that has damaged or pinched a nerve can often be addressed surgically. Damaged muscles or tendons in the leg or foot can also be repaired in surgery. Patients suffering from persistent or chronic foot drop that is resistant to treatment may benefit from surgical intervention that fuses the bones of the ankle or foot, or even surgery that transplants and/or reconfigures tendon and muscle.
Functional electrical stimulation (FES)
In cases where peroneal nerve damage or impairment is causing foot drop, functional electrical stimulation (FES) can be an effective form of treatment. Therapeutic FES treatment in conjunction with physical therapy can help stimulate damaged nerves and muscles and promote motor recovery.
FES treatment uses sophisticated equipment to deliver targeted pulses of electrical current that evoke muscle contraction and activity. This can improve muscle functionality, enhance blood flow and range of motion, reverse muscle atrophy, and—in some cases—help foot drop sufferers regain some or all of their ability to lift their foot/feet and walk normally. Portable FES devices designed specifically for foot drop patients are also available. These systems deliver low-level FES impulses targeting the peroneal nerve, allowing wearers to achieve improved foot dorsiflexion and walk more naturally—with improved speed, stability, and confidence. These two-part systems use a specialized sensor to monitor the motion and position of the leg, in conjunction with a stimulator that delivers the electrical impulse and stimulates the peroneal nerve.
Physical therapy
Physical therapy is an important and often effective treatment option for foot drop that can be used alone or in conjunction with another treatment. The overall goal of any therapeutic or rehabilitation program for foot drop is to strengthen the muscles in the foot, ankle, and lower leg, enhance joint function and range of motion, prevent stiffness, minimize the chances of re-injury, improve balance and stability, and ultimately achieve improved mobility and regain a normal gait.
While the specific details of a therapy program for foot drop symptoms may vary from patient to patient, strength and balance training, stretching, and range of motion exercises are standard. Exercises include stretching with towels or exercise bands, seated or standing lifts, ankle dorsiflexion and plantar flexion exercises (pulling the foot toward you and pushing it away from you) with resistance from exercise bands, and even picking up small objects with your toes.
Foot drop patients should participate in a personalized therapeutic program under the guidance of a physical therapist with demonstrated experience working with foot drop patients. While in-office visits and therapy sessions are critical, most programs also include a home component with a series of exercises that the patient can perform independently.
External support and bracing
After determining the root cause for the foot drop and beginning a therapy program that incorporates the many facets of therapeutic care, including strength training, range-of-motion stretches, balance training, etc, the next step involves orthotic treatment to improve function and safety while reducing the risk of joint damage until the patient has fully recovered. An ankle-foot orthosis (AFO) can help to stabilize the affected foot and help foot drop patients maintain a normal foot position.
It is highly advisable that doctors and therapists who frequently see patients with foot drop take the time to establish a good working relationship with an orthotist. That relationship is the key to ensuring a collaborative, multidisciplinary approach where the patient, the therapist, and the orthotist are all on the same page.
Patient Safety
The highest priority of orthotic care is patient safety. Safety can be greatly improved by use of an AFO by restricting or reducing plantar flexion during swing phase of gait, and thereby reducing the risk of a fall due to catching the toes on the ground. Without the use of an AFO, many gait deviations are utilized to clear the foot during swing phase, including circumduction, hip hiking, and contralateral vaulting. These deviations increase the energy expenditure of the gait and can create muscle imbalances that often lead to further issues and complications.
Early Intervention
Early orthotic intervention is also beneficial for reducing the risk of joint contractures in patients with increased tone, such as a post-CVA foot drop with resulting equinovarus foot position. The AFO can properly position the foot in the coronal and sagittal plane to help maintain functional joint range of motion.
Innovations and Options
Revolutionary changes have taken place in the orthotic industry in the past 20 years. New lightweight materials have been introduced that are not only supportive, but can also provide energy storage and return to assist with push-off at terminal stance for patients with weak calf muscles.
When determining what kind of orthosis would provide the optimal treatment for a foot drop patient, one concept should always be remembered: joint motion should be permitted in an orthosis when sufficient muscle control and strength are present to move the joint normally through the available range. What this means is that, while support is crucial, “overbracing” a patient can create many negative consequences; some of which include muscular atrophy, dependence on the orthosis, and replacing one gait deviation with another by taking away the essential three rockers of gait. It is essential that when a patient has sufficient strength to control the ankle joint in a certain motion, that the orthotic allows them to do so.
One example of overbracing would be putting a patient with a flaccid foot drop (weak dorsiflexors) but strong plantar flexors into a solid ankle AFO. This AFO solution would prevent them from using their calf musculature at terminal stance for push-off. It also would prevent anterior tibial translation during the second rocker of gait, creating an unsmooth rigid transition through mid-stance. That could subsequently lead to genu recurvatum by restricting dorsiflexion of the ankle. A more appropriate AFO selection may be something with flexibility that has enough plantar flexion resistance to improve clearance of the foot during swing phase, but also lets the patient use their own musculature for other motions that they can control appropriately.
Manufacturers provide plentiful options to the physical therapy market for off-the-shelf and custom AFOs. Rockaway, NJ-headquartered Allard USA offers AFOs designed especially for foot drop that provide mild, moderate, and maximum stability. The company’s ToeOFF is a carbon composite dynamic response floor reaction AFO designed to keep the foot up during swing phase and provide a soft heel strike in addition to stability in stand and good toe-off. The company also offers the ToeOFF and the BlueROCKER as custom AFOs when more specific needs must be met, such as fit issues related to unique leg shapes, alignment issues, or calf atrophy/hypertrophy.
Another manufacturer, DJO Global, Dallas, offers a line of AFOs including the lightweight Posterior Leaf Splint AFO, designed to provide utility for mild to moderate foot drop needs. Cascade Dafo Inc, Ferndale, Wash, offers a versatile line of pediatric dynamic AFOs that are available as customized products and feature colors and design elements that will appeal to children.
Ongoing Consultation
As recovery progresses, the orthotist should be consulted on a regular basis so that the AFO can be changed or modified throughout each stage of rehabilitation. As the patient’s condition changes, the therapeutic remedies (from exercises to AFO solutions) should change with them. The ultimate goal is to eventually eliminate the need for the brace entirely, because full function has been regained. In the meantime, the proper orthosis can be very beneficial in improving function and safety until independence is possible without it. PTP
Polly Swingle, PT, GCS, CEEAA, is co-founder and lead physical therapist of The Recovery Project, which provides progressive, effective, evidence-based neuro rehab therapies that improve the quality of life and functionality of patients with spinal cord, neurological, and traumatic brain injuries at its three Michigan-based locations.
Brian Paulson, CPO, is a clinical manager for Wright and Filippis, a Michigan-based provider of prosthetics, orthotics, custom mobility products, and accessibility solutions with over 70 years of experience. For more information, contact PTPEditor@medqor.com.